Goal-setting/Determination of Intervention Targets

Setting Goals Oriented Toward Independent Living
To achieve this new service-program goal Martin and his rehabilitation team set short-term cycle goals i.e. ‘vocational reintegration’, ‘independent mobility and housing’, ‘recreation and leisure’, and ‘optimised motor functioning’ corresponding to cycle goal 1, 2, 3 and 4 respectively. Achieving this service-program goal served as another step toward meeting Martin's global goal of independent living. All of these goals were documented in the ICF Categorical Profile, a visual depiction of a person's functioning status at the time of assessment showing the qualifier values for selected ICF categories considered relevant to the person's case.
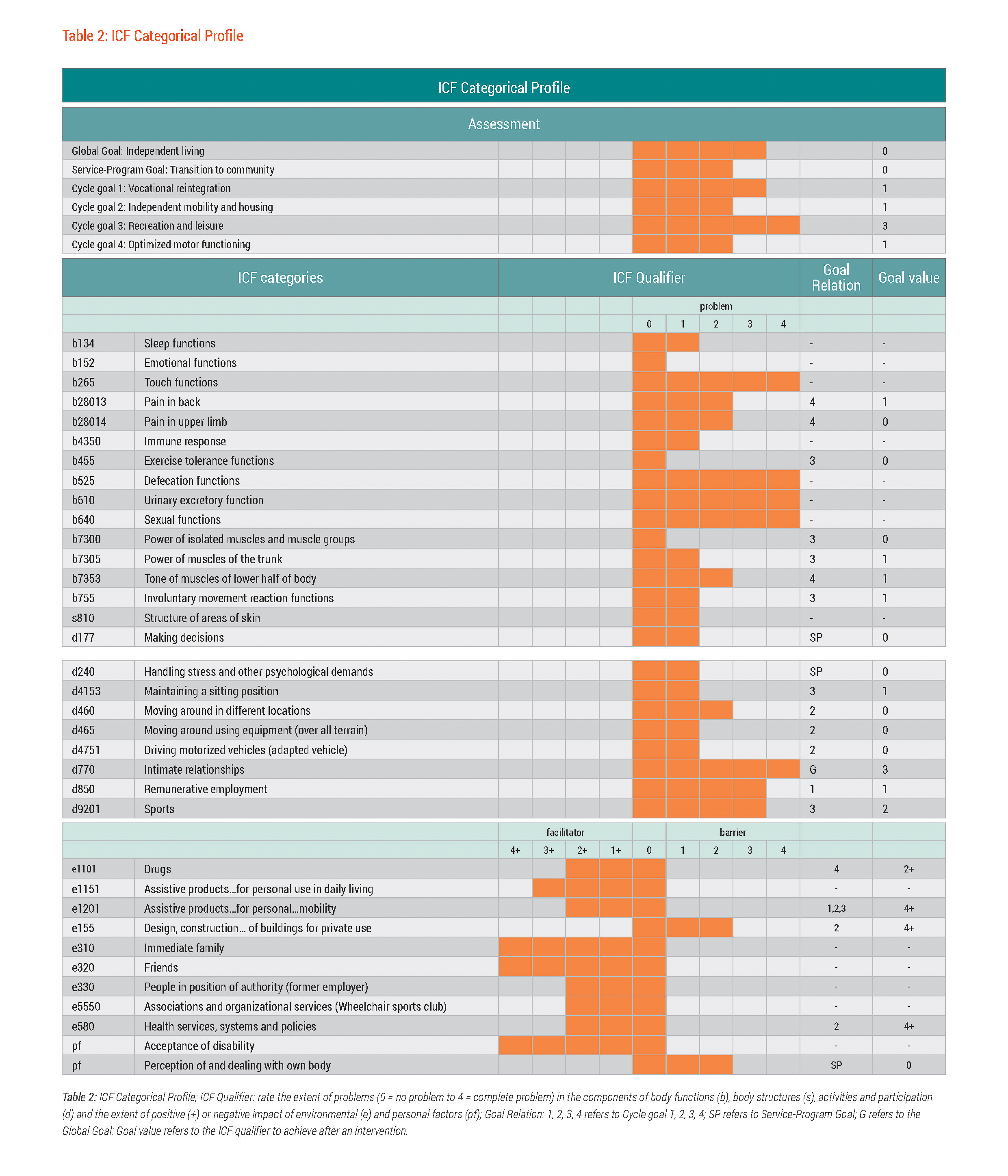
Table 2: ICF Categorical Profile; ICF Qualifier: rate the extent of problems (0 = no problem to 4 = complete problem) in the components of body functions (b), body structures (s), activities and participation (d) and the extent of positive (+) or negative impact of environmental (e) and personal factors (pf); Goal Relation: 1, 2, 3, 4 refers to Cycle goal 1, 2, 3, 4; SP refers to Service-Program Goal; G refers to the Global Goal; Goal value refers to the ICF qualifier to achieve after an intervention.
The cycle goals reflected the issues that Martin and his rehabilitation team felt were essential to address in order to ensure success in independent living and community reintegration. These issues were:
- Employment – To build upon the gains from the vocational rehabilitation (VR) efforts in Martin's first Rehab-Cycle®, and to clarify Martin's potential avenues for employment
- Housing – To clarify the availability of accessible and desirable housing
- Mobility – To be independent in manoeuvring the wheelchair in any location, as well as in driving and using various means of public transportation
- Recreation – To identify Martin's interests in recreation and leisure activities in addition to sports, and to clarify the availability of accessible sporting and other recreational activities in his home community
To advance vocational reintegration (cycle goal 1), Martin's decision-making competencies still needed improvement, suitable career options had to be identified, and ensuring employer support was vital for concrete planning of Martin's vocational future.
Achieving cycle goal 2 ‘independence in mobility and housing’ was multi-fold. Becoming independent in mobility required further wheelchair training on a variety of terrain, training on driving an adapted car, and securing the required license for driving an adapted car. Assistive devices such as a Swiss-Trac™ and an adapted car had already been ordered, but cost coverage had still not been confirmed by the insurance company. With regard to housing, it was essential that Martin funnel his decision-making competencies and the energies harboured in stress toward finding a suitable place to live.
In order to facilitate Martin's participation in sporting and other recreational and leisure activities (cycle goal 3), Martin's exercise tolerance, muscle and movement functions, and the ability to maintain a sitting position had to be improved. In addition, contact with a local sports club for the disabled had to be initiated.
Fundamental to achieving success in cycle goal 4 ‘optimised motor functioning’ was strengthening Martin's immune response to various irritants and pain management. For example, Martin often experienced increased spasticity and muscle stiffness as a response to recurring urinary tract infections. Managing pain would help increase Martin's range of motion, and would enable him to intensify physical training. Moreover, helping Martin to perceive his body in a more positive light was expected to contribute to the optimisation of his motor functioning.
For each of the cycle goals intervention targets were established. Intervention targets are ICF categories outlined in the ICF Categorical Profile that correspond to goals set and are intended to be addressed with specific interventions. The intervention targets and the corresponding goals identified for Martin, as well as the interventions provided in the last weeks before his discharge follow the spirit of the transitional rehabilitation approach. See box 2 below.
Box 2 | The Transitional Rehabilitation Approach12
The transition of a person with spinal cord injury (SCI) from a hospital or rehabilitation centre back to his or her community marks a major milestone in the rehabilitative process and in the life of the individual. In addition to the sudden discontinuity of service upon discharge, and the often lengthy stay in a traditional inpatient rehabilitation setting – sometimes characterized by the isolation from family and friends, an artificially regulated environment, periods of non-productive time alone, and the adoption of a dependency role – can contribute to psychosocial difficulties a person faces after discharge, including decreased community participation. Moreover, the services available in the community tend to be fragmented, thus further impeding the successful transition to the community.
To counter the negative impact of often ineffective community integration planning in traditional rehabilitation settings, transitional rehabilitation programs (TRP) have been developed. The TRP approach is intended to bridge primary inpatient rehabilitation and tertiary community rehabilitation. TRP begins before discharge and takes place primarily in the person's home or in a home-like environment away from the hospital setting. It aims to reduce the time spent in the hospital, ensure continuity of care from the inpatient setting to community setting, reduce fragmentation of service provision, increase a person’s control over his or her own rehabilitation, and ultimately enhance community reintegration.
Once a transitional rehabilitation approach is decided on, the person and the multidisciplinary rehabilitation team develop a mutually agreed individualised TRP plan that includes concrete goals and the interventions and strategies to achieve these goals. The TRP plan is flexible and can be modified according to the person's evolving situation. Issues that are generally addressed through TRP interventions include, but not limited to housing, mobility, transportation, acquisition of assistive devices and equipment, interpersonal relationships and sexuality, and employment.
The complex and multidisciplinary nature of TRP interventions necessitates that each stakeholder in the process is invested and actively involved. Not only do the rehabilitation professionals provide the respective services and establish supporting links to community resources, the person must also take an active role in finding community resources and establishing community links, and take the lead in re-establishing his or her role in the family and society. In addition, the person’s family needs to be adequately prepared and included in the transition process.
From a systems perspective, the transitional rehabilitation approach is seen as process- and outcomes-oriented and as a possibility for reducing health care costs, shortening hospital stays, decreasing re-admission rates, and improving long-term outcomes of those undergoing transition to the community.