General Introduction

In consideration of available (including historical) conceptualisations of the term “stress", two pioneers of research on stress and coping, Richard Lazarus and Susan Folkman defined (psychological) stress as “a particular relationship between the person and the environment that is appraised by the person as taxing or exceeding his or her resources and endangering his or her well-being”.1. This definition takes into account the personal factors of the individual who is experiencing stress as well as the nature of the stress-producing event. It also emphasises that the experience of stress depends on how the person perceives the event.
""SCI is a stress-producing, life-changing event.""
Experience of Stress after SCI
SCI is a stress-producing, life-changing event.2345 Stressors i.e. stress stimuli or stress-producing environmental events1 that may cause a person with SCI to experience stress include the inability to perform activities equally well as before the injury, social demands e.g. work, obligations of family and friends, and the physical changes associated with SCI.678
Other stressors that can also impact a person's psychological well-being include (but are not limited to) pain, fatigue, medication, isolation, medical complications, body image, dependency, feelings of helplessness and humiliation, and cognitive problems.8910
Response to Stress after SCI
The response to stress or various stressors vary among persons and over the course of recovery; it can also fluctuate during a person's course of life.6 An early emotional reaction to SCI can be denial, a reaction that prevents a person from confronting the dramatic changes that he or she is faced with. This may be followed by other responses such as anger, sadness or even depression, anxiety and grief.4589
""How a person’s responds to stress/stressors is associated with coping.""
How a person’s responds to stress/stressors is associated with coping. Coping can be viewed as "a protective factor that facilitates adaptation to stressful life events”.11 A number of studies have demonstrated that coping is an important mediator of a person's emotional adjustment to SCI.26
Box 1 | Coping
In line with their definition of stress, Lazarus and Folkman defined coping as “constantly changing cognitive and behavioural efforts to manage specific external and/or internal demands that are appraised as taxing or exceeding the resources of the person”.1 This definition indicates that coping is a process that requires some sort of effort as a reaction to psychological stress, and encompasses what the person thinks or does in order to manage (minimise, avoid, tolerate, accept, master) the stressful situation.
According to Lazarus and Folkman there are two forms of coping:1
- Emotion-focused coping – strategies that focus on regulating the emotional response to psychological stress and are often employed where the person feels that he or she has no control over the situation
- Problem-focused coping – strategies directed at managing or changing the source of stress and are often employed where the person sees the situation as controllable
Emotion-focused coping includes a spectrum of strategies including (but not limited to) venting of emotions, acceptance, positive reappraisal, avoidance, wishful thinking, distancing, and denial.126 Research has shown that persons who employ certain emotion-focused coping strategies, such as venting emotions, experience more depression and anxiety than those who employ active problem-focused coping strategies. On the other hand, emotion-focused coping such as acceptance and positive appraisal have shown to be associated with reduced psychological stress among persons with SCI.2 In general, problem-focused coping is seen as more favourable; the use of these strategies have shown to lead to lower psychological problems and to a more positive mood. The degree to which each of these strategies is employed may change over time, and will depend on the person's personal factors and nature of the stressor.12467
These two forms of coping are integral elements of Lazarus and Folkman's model of stress, appraisal and coping. The original stress, appraisal and coping model has evolved to include the aspect of positive emotion and meaning-focused coping. These additional elements were introduced to the model to show what could happen after the two forms of coping are applied and the outcome is unfavourable.112 See figure 1.
BITTE DIESE ABBILDUNG MIT DER NEUEN FIGURE 1 ERSETZEN
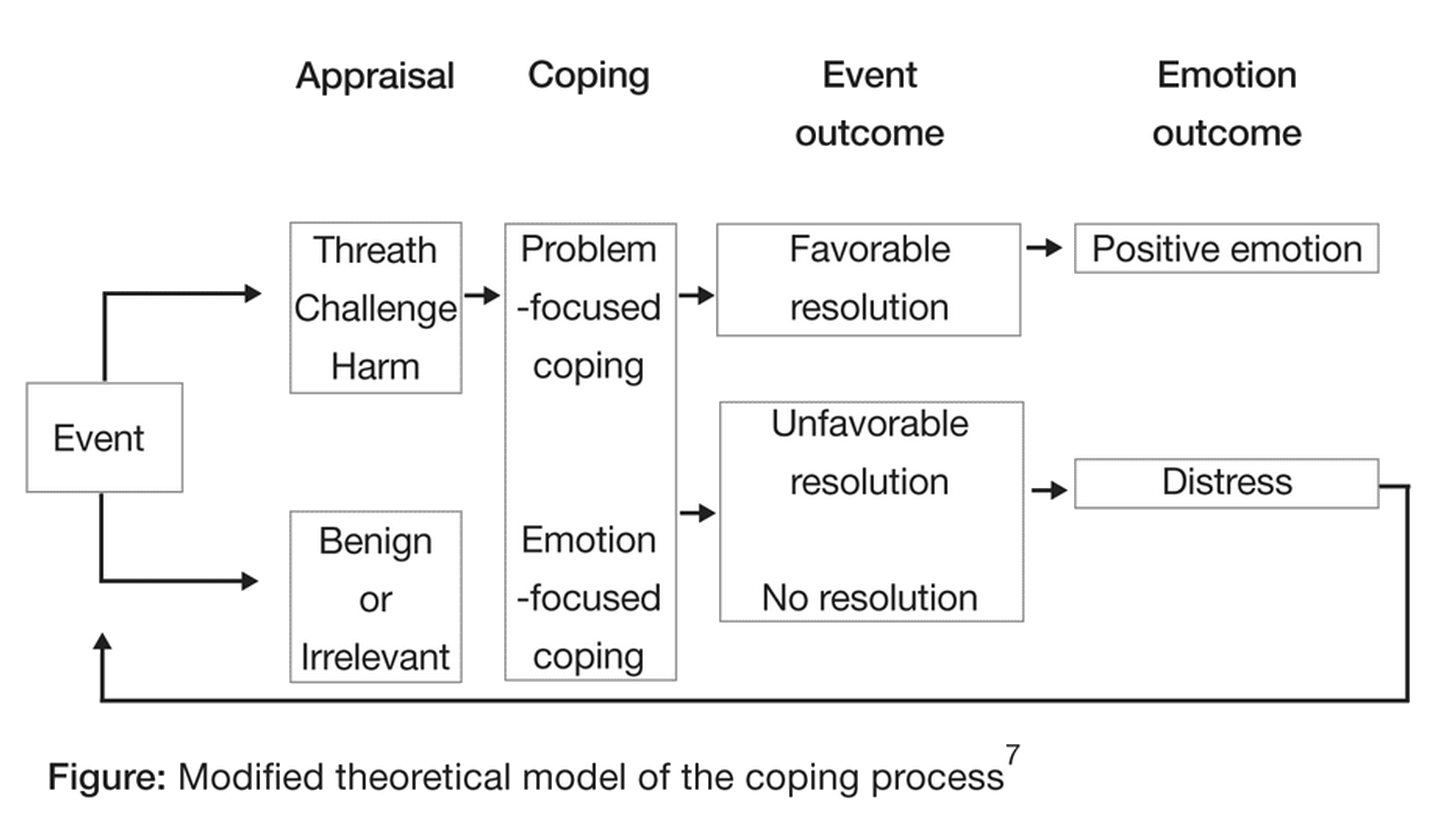
Figure 1. Revised stress, appraisal and coping model12
Basically, meaning-focused coping can help a person deal with an unfavourable outcome by drawing upon his or her beliefs, values, and goals. Meaning-focused coping could include searching for and finding possible benefits in a particular situation, pursuing goals as a means for developing a sense of purpose, reordering of priorities to adapt to changed realities, and focusing on the positive aspects of life. In turn, such meaning-focused coping can trigger positive emotions; positive emotions have been shown to play a significant adaptational role in the stress and coping process.12
As the name of the model implies, an essential element of the stress, appraisal and coping model is appraisal i.e. how the person perceives the stress he or she is experiencing. The person's appraisal of a stressor and the resources available for dealing with it can determine the coping strategy he or she employs.12121314
""...while persons with SCI have a greater risk for depression and anxiety, these disorders are by no means inevitable outcomes of SCI.""
Post-SCI stress can lead to psychological disorders, including depression and anxiety.5 It had been previously thought that depression, for example, was an inevitable consequence of SCI. However, while depression is commonly reported by persons with SCI, most often occurring early following injury, there is no empirical evidence that a person with SCI will inevitably experience depression, and the majority of persons with SCI do not develop it.451317141819 Nevertheless, since depression and anxiety are the main psychological disorders faced by persons with SCI, it would be important to highlight some relevant information about depression and anxiety in SCI.
Box 2 | Depression and Anxiety in SCI
Depression
Depression is a range of disorders that includes adjustment reactions with a depressive mood and major depressive disorder. A brief or short-term experience of sadness does not necessarily equate with depression. Studies have found an increased prevalence of depression i.e. 20-45% in adults with SCI compared with the general population. The occurence of depression in persons with SCI does not seem to be directly linked with the level of injury or whether the SCI is complete or incomplete, but rather stem more from the stressors the person experiences following SCI. Pain, feelings of helplessness and lack of control seem to be predictors of depression. In addition, the risk of developing depression is higher for those with pre-SCI substance abuse and depression, as well as family history of depression and suicide. Moreover, SCI has shown to be associated with increased hospitalisation and SCI-related secondary complications, and a higher risk of premature mortality in persons with SCI.4514171819
Anxiety Disorders
Described as disorders involving real or imaginary perceptions of tension, worry, fear and vulnerability, anxiety disorders can include generalised anxiety disorder, social anxiety, acute and post-traumatic stress disorders (PTSDs).5 Persons with SCI who also have an anxiety disorder may experience fear of death or of living with medical complications and disability, may worry about loss of independence, financial stability, and control, etc., about physical appearance, and about losing love from friends and family.58
Various studies have found that the prevalence of anxiety disorders in persons with SCI is 16-30%. PTSD, a specific anxiety disorder, has shown to have an incident rate that varies between 5-50% and a prevalence rate between 7-61%.2568918
Given the elevated prevalence of depression and anxiety disorders after SCI, it would be essential to address these and other mental health issues in rehabilitation.45613141819
Rehabilitation Interventions
In the rehabilitation of persons with SCI, health professionals have the important task of fostering the person's adjustment to their post-SCI situation and the development of successful coping strategies. With regard to depression, research has shown that the way persons with SCI cope with their injury early in their rehabilitation predicts the extent of depression experienced later.13 Results of a 2016 published 21-year longitudinal study suggest that psychological interventions to address depression could reduce the risk of depression and pre-mature mortality in persons with SCI.14 Thus, early screening and assessment, and timely management of depression are vital.414
Interventions to manage depression and other mental health issues, and to promote adjustment following SCI are multi-faceted; determining the appropriate intervention(s) can be difficult.18 Interventions can include education, providing information on available support services and resources, psychological counselling, medication, peer mentoring and support, and ongoing long-term monitoring.45 14
Since SCI also has implications for the family of the person living with SCI e.g. changing roles, impact on sexual relationships, promoting the physical, social and emotional health of family members through support and interventions is also important.45
""...early screening and assessment, and timely management...are vital.""
Rehabilitation interventions, especially psychological counselling and cognitive behavioural therapy, played a crucial role in this case study of Ingrid, a 37-year old woman who sustained a SCI following a mountain bike accident. The case will illustrate how Ingrid's experience of stress impacted on her psychological well-being and the challenges the rehabilitation team faced in their efforts to promote her psychological well-being, while highlighting the importance of individual coping strategies in the rehabilitation process.